If you experience a sudden and severe headache, be careful! It could be an intracranial aneurysm. An intracranial aneurysm is the ballooning of a weakened blood vessel in the brain, which causes an intense headache upon rupturing. Around 3% of the population have unruptured aneurysms, which should be treated before they rupture. In 2011, Aoki’s group at Kyoto University suggested that nonsteroidal anti-inflammatory drugs (NSAIDs) may be an alternative to surgical repair, which is currently the only treatment for aneurysms.
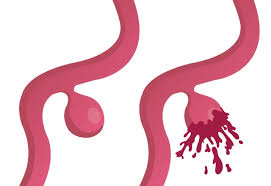
Unruptured aneurysm (left) vs. Ruptured aneurysm (right)
(Credit: Mayo Clinic)
Mechanism of NSAIDs
Inflammation leads to the growth and rupture of intracranial aneurysms, but NSAIDs reduce inflammation by inhibiting the cyclooxygenase (COX) enzymes, specifically the COX-2 pathway. When this pathway is activated by inflammatory stimuli, the COX-2 enzyme converts arachidonic acid to prostaglandin, which then upregulates sequential reactions to promote inflammation, and enlarges intracranial aneurysms. Aoki’s team observed that NSAIDs decreased the formation of intracranial aneurysms in mice within the first six weeks.
Risks associated with NSAIDs and surgical repair
Although this treatment seems promising, long-term use of NSAIDs may lead to cardiovascular and gastrointestinal side effects. There are two surgical options to treating aneurysms: endovascular coiling and clipping. A major risk for coiling is that it may develop vasospasm, which occurs when the vessel constricts and leads to tissue death; whereas clipping increases the risk of infection and death, as it is an open surgery.
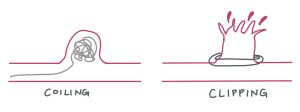
Two surgical procedures: Coiling an unruptured aneurysm (left) vs. Clipping a ruptured aneurysm (right)
(Created with Notability)
Both surgical and potential pharmacological treatments come with their risks, but hopefully our advancing knowledge will soon bring forth safer therapies.
Athena Wang
