We are constantly encountering pathogens (anything that can cause disease), so why don’t we become sick more often?
The answer to this question is our immunes system, which is responsible for protecting us from diseases.

The immune system
Credit: In a nutshell – Kurzgesagt
From a scientific point of view, the immune system includes many biological structures and processes that an organism has in order to response to diseases that come from bacterial or viral infections.
The immune system reacts to diseases with layered defenses of increasing specificity. There are two lines of defenses in our body: 1- innate defenses, 2- adaptive defenses
The innate defenses include two major parts. In the first part, there are physical barriers such as a tough outer skin, mucous membranes and secretions that are all impenetrable to viruses and bacteria. In the second part, which is more detailed, body protects itself by phagocyctic cells and natural killer cells, which are white blood cells. In addition to these white blood cells, complement proteins and the inflammatory response (swelling, fever and redness) also play important roles in this kind of defense.
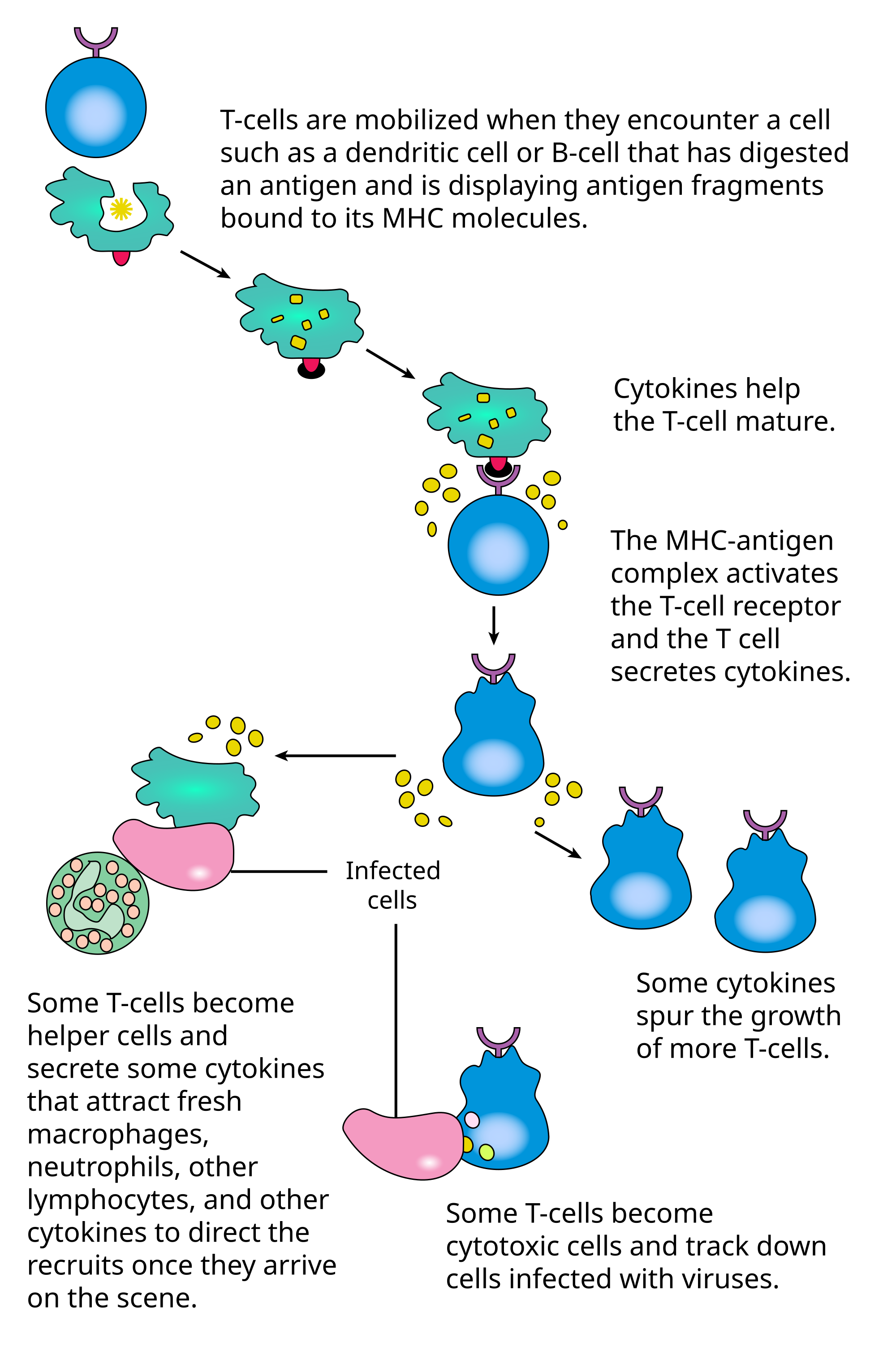
After innate defenses, there is a more specific line of defense, which is called adaptive immune response. This kind of defense provides immunity against particular pathogens that the innate immune response is not able to kill and remove them. T cells and B cells are lymphocytes that play the most important role in the adaptive immune response.
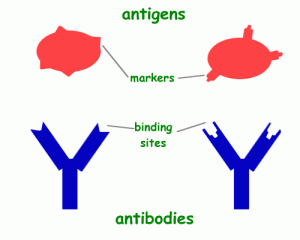
B cells respond to presence of pathogens by recognizing them, secreting antibodies which are types of proteins that bind to pathogens and inactivate them and create the memory of them.
The last part of the adaptive immune response is T cells. These cells have receptors on their surface and use them in order to recognize infected cells, kill invaders and stimulate more B cells.
Kamyar Kazemiashtiani