Three Cases of “Flesh-eating”
Bacterial Infections in Hong
Kong
.
.
Three cases of necrotizing fasciitis— an infection caused by bacteria that destroys skin, fat, and the tissue covering the muscles in a short period of time—have been reported in Hong Kong during the month of July in 2015. Similar sporadic cases have also been reported in April and August of 2015 in Hong Kong. The affected include: an 82-year-old man and 78-year-old woman with underlying chronic illnesses and a 59-year-old man with good past health.
The causative agent is a rare but deadly pathogen, Vibrio vulnificus and its name literally translates to “causing wounds” in Latin. V. vulnificus is one of the three major species of Vibrio, with the other two being V. cholera and V. parahaemolyticus both of which are pathogens of humans.
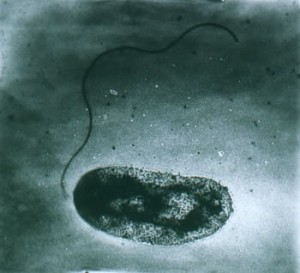
V. vulnificus is a Gram-negative, lactose-fermenting, opportunistic (similar to L. monocytogenes), and motile curved bacterium commonly found in marine and estuarine environments. It is a moderate halophile (requires salt for growth) and is frequently isolated from oysters, clams, crabs, and other shellfish in warm coastal waters. It is responsible for causing 95 percent of all seafood-related deaths and has a mortality rate of over 50% in North America. The mortality rates varied in Hong Kong, being 35% for septicaemia cases and 20% for wound-infection cases.
V. vulnificus has the ability to cause wound infections, gastroenteritis, or a syndrome known as primary septicemia. Infections among healthy individuals are acute and do not have long-term consequences; ingestion of this bacterium causes mild symptoms such as vomiting, diarrhea, and abdominal pain usually within 16 hours.
In the immunocompromised population however, V. vulnificus can trigger further complications and has the potential to invade the bloodstream from an open wound or from the gastrointestinal tract, causing primary septicemia – a severe and life-threatening illnesses. This disease is characterized by fever, chills, septic shock that is soon followed by death. The three patients affected in Hong Kong had to either undergo amputation or excisional debridement.
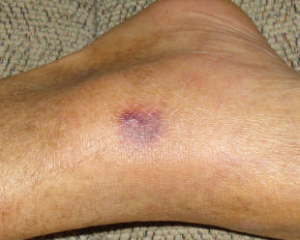 (There are much worse pictures than this one!)
(There are much worse pictures than this one!)
Individuals are considered high-risk and vulnerable to infection if they have underlying chronic diseases or liver diseases [i.e. diabetes, cirrhosis, leukemia, lung cancer, acquired immune deficiency syndrome (AIDS), AIDS- related complex (ARC), or asthma requiring the use of steroid]. They are 80-200 times more likely to develop primary septicemia than healthy individuals.
The infective dose for healthy individuals is unidentified but for immunocompromised persons, septicemia occurs with doses of less than 100 total organisms. The incubation period is 1 – 7 days after eating and the duration of illness ranges from 2 to 8 days. Diagnostic methods are similar to those used to detect common foodborne pathogens and revolve around culturing of the organism from wounds, diarrheic stools, or blood. Methods such as the Quantitative Loop-Mediated Isothermal Amplification can quantitatively detect V. vulnificus in raw oysters with high speed, specificity, and sensitivity.
Measures that can be taken to prevent illness include:
• Avoid going into the ocean with open wounds (I think most people neglect this)
• Avoid eating raw or undercooked shellfish
• Before cooking: Discard any oysters with open shells
• During cooking: Boil for 3-5 minutes after shells open.
• After cooking: Discard any oysters with shells that did not open.
There have been many sporadic cases of V. vulnificus in Hong Kong over the past decade. Although the Centre for Health Protection of Hong Kong offers various Internet resources on how to prevent V. vulnificus infections, many of the victims are the elderly and are less likely to be able to access this information. I believe that more focus needs to be directed to relaying information on opportunistic foodborne pathogens to the elderly and immunocompromised in a manner that is not via the internet, i.e. various clinics and hospitals should offer them pamphlets and communicate with them verbally. In 2013, Health Canada has collaborated with the FAO, WHO, and the government of Japan to produce expert recommendations to the Codex Committee on Food Hygiene regarding V. vulnificus. Appropriate methods to monitor environmental hygiene and hygienic production, etc. can be found in Codex Alimentarius Guidelines on the Application of General Principles of Food Hygiene to the Control of Pathogenic Vibrio Species in Seafood.
Questions for thought:
1. Is this pathogen present in other geographical areas?
2. Which method(s) would be most suitable to detect the presence of this pathogen based on it transmission route?
References:
Codex Alimentarius (2010). International Food Standards. Guidelines on the Application of General Principles of Food Hygiene to the Control of Pathogenic Vibrio Species in Seafood. Retrieved from: http://www.codexalimentarius.org/standards/list-of-standards/
FDA (2015). Vibrio vulnificus. Bad Bug Book: Foodborne Pathogenic Microorganisms and Natural Toxins Handbook. Retrieved from: http://www.fda.gov/Food/FoodborneIllnessContaminants/CausesOfIllnessBadBugBook/ucm070473.htm
Han, F., Wang, F., & Ge, B. (2011). Detecting potentially virulent vibrio vulnificus strains in raw oysters by quantitative loop-mediated isothermal amplification. Applied and Environmental Microbiology, 77(8), 2589-2595.
Lee, S. E., Kim, S. Y., Kim, S. J., Kim, H. S., Shin, J. H., Choi, S. H.. . Rhee, J. H. (1998). Direct identification of vibrio vulnificus in clinical specimens by nested PCR. Journal of Clinical Microbiology, 36(10), 2887-2892.
Ma, J (2012). Vibrio vulnificus in food. Food Safety Focus, 72. Retrieved from: http://www.cfs.gov.hk/english/multimedia/multimedia_pub/multimedia_pub_fsf_72_01.html
Stone, J. (2015). With Global Warming, Expect More Deadly Vibrio Cases. Pharma & Healthcare. Forbes. Retrieved from: http://www.forbes.com/sites/judystone/2015/07/30/with-global-warming-expect-more-deadly-vibrio-cases/
Treasury Board of Canada Secretariat (2015). Food and Consumer Safety Action Plan. Retrieved from: https://www.tbs-sct.gc.ca/hidb-bdih/plan-eng.aspx?Org=0&Hi=85&Pl=403
Vibrio vulnificus (2013). Vibrio Illness (Vibriosis). Centers for Disease Control and Prevention. Retrieved from: http://www.cdc.gov/vibrio/vibriov.html
elaine chan 3:37 pm on November 14, 2015 Permalink |
Definitely an interesting, yet scary article! Commonly, food illnesses are related to gastrointestinal diseases, it’s my first time seeing how it can also lead to wound formation, and subsequently amputations and excisional debridements! This is definitely a wake up call for the food and marine industry to ensure the safety of their products for consumers. To determine whether or not this pathogen can be found in other geographical areas, I think it will be important to determine the pathogen’s favourable growth conditions and then evaluate which geographical areas has the potential of promoting the growth of such pathogen.
csontani 3:46 pm on November 14, 2015 Permalink |
This is definitely interesting to read! I’ve never heard of this pathogen before and it’s scary knowing what it can do to you. After reading this, the first question that popped in my mind was “is this pathogen a concern in where I’m currently living at?”. I certainly agreed with what you said regarding how the health agency should focus on older citizens who are immunosuppressed since they’re less likely to check the internet regarding the foods they’re eating. Maybe the food product packaging could have more information regarding the food and risks it may content or maybe health agency could talk to the senior care centre to give informations regarding these kinds of concerns.
angel519 10:24 pm on November 14, 2015 Permalink |
Since we live at the coast where we also consume oysters, clams, crabs, and other shellfish, and we also consume imported shellfish from warm coastal water; it is a potential pathogen that could be present at B.C. I think it is necessary to have warnings and publicize the risks of consuming contaminated shellfish to the general public. And for the high-risk population, especially the elderly, grocery stores can have brochures and signs by the shellfish section to tell them how to properly cook shellfish, symptoms of infections and to seek doctors if feel unwell after consumption. It is also important to have regular inspections on shellfish to prevent infected products spreading in the market.
Jasmine Lee 1:35 am on November 15, 2015 Permalink |
This pathogen is by far the most frightening of those that I have come across in this class. It is interesting to learn about a pathogen that thrives in environments with high salt levels. This is concerning since high osmolarity and low water activity are commonly used as hurdles for food safety and bacterial control. I also found it surprising that gender may play a role in regards to the pathogenicity of the V. vulnificus’ toxin. An article claimed that estrogen may assist in protecting against endotoxic shock and lowering the risk of mortality in individuals (Merkel et al., 2001). Furthermore, I agree with Angel that regular inspection of shellfish products and consumer awareness are critical for lowering the risk of exposure. It is also important to post signs along coastlines and have restaurants alert consumers about the associated risk with eating raw seafood. With many biological hazards in raw foods, I hope consumers are more diligent in terms of ensuring food safety and will make informed decisions for themselves.
Merkel, S.M., Alexander, S., Zufall, E., Oliver, J. D. and Huet-Hudson, Y. M. (2001). Essential role for estrogen in protection against Vibrio vulnificus-induced endotoxic shock. Infection and Immunity, 69(10):6119-6122.
Susanna Ko 9:28 am on November 15, 2015 Permalink |
I find this article really scary because I can see my parents falling victim to this. There’s a lot of canned seafood products (clams, oysters) on the market. Cuisine with oysters is probably very popular as well. My parents like to add canned oysters into their congee. Perhaps popular asian newspapers should have a food safety section. I know my parents will probably read it.
cheryl lau 3:20 pm on December 4, 2015 Permalink |
This was a very scary article to read! However, I think it is necessary to point out the dangers we face when we expose ourselves to harmful microorganisms. Even though our bodies have defenses in place to fight invaders, they may not be as sound as we think. In this case, V. vulnificus caused serious consequences. I feel that most people in Hong Kong do not realize the serious affects that could follow from eating contaminated seafood. Specifically, the elderly or the people from our parents’ generation may not have been educated in food safety and I think these issues should be more prominent in the media.
EmilyLi 9:40 pm on December 13, 2015 Permalink |
This is a very interesting yet scary article to read. I think you title is very eye catching too. I personally like to eat seafood, and especially if you travel to coastal city like Hong Kong how could you resist the seafood there. Although in the article it mention that the pathogen is only high risk for immunocompromised individuals. However, with knowing that you are infected with a pathogen that is likely to breakdown flesh in your body is quite scary. Especially when you could catch those with just wound on you legs and going to the beach.
EmilyChow 3:25 am on December 15, 2015 Permalink |
It’s scary to think about these cases because they could potentially also happen here on the west coast of North America! This bacteria can possibly survive in pacific water conditions and contaminate the seafood we have here. In addition, seafood is imported and exported around the world so this is a concern for international seafood lovers. Since seafood can be enjoyed in different ways (canned, cooked, raw), it’s important to have strict processing regulations and make sure that such regulations apply for all pathogens, considering V. vulnificus is relatively rare.